Posterior prolapse happens when your rectum begins poking through the wall that separates it from your vagina. It can be a painful condition, but sometimes, you don’t know you have rectocele until your Brooklyn gynecologist discovers it during a routine exam. At one of the Century Medical and Dental Center offices, you can find effective treatments from physical therapy to surgery. Call today for an appointment.
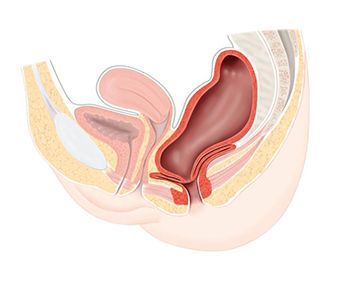
Pelvic prolapse refers to a condition in which any of your pelvic organs push through weakened pelvic floor muscles. Rectocele — also called posterior prolapse — involves the specific condition when the barrier of tissue between your vagina and rectum thins or weakens to the point that the rectum bulges into or through the vaginal wall. Mild cases of posterior prolapse usually cause little or no symptoms, but if the prolapse progresses, the rectum descends further, and symptoms become stressful, embarrassing and painful.
While tissues separating the vagina and rectum tend to weaken as you age, other conditions can strain them. Childbirth, injury, chronic constipation and even habitual, violent coughing contribute to weakening muscles. Nonsurgical treatment options exist, although severe prolapse conditions may require a surgical intervention.
Minor posterior prolapses usually cause little or no discomfort or symptoms. If it descends further, you may notice:
Rectocele often accompanies other pelvic prolapse conditions involving the bladder, uterus, or the top of the vagina. Although childbirth often contributes to posterior and pelvic prolapse conditions, women who haven’t had children may experience them as well.
Women carrying pregnancies to term, complete with vaginal childbirth, especially of babies nine pounds or heavier, often develop prolapse conditions later in life. Other causes include:
Individuals who have dealt with sexual abuse as a child may experience more trouble with pelvic prolapse conditions. Reduced estrogen weakens the pelvic lining and muscles. By the age of 50, about half of all women have some signs of pelvic prolapse. Some researchers suggest that women who’ve had chronic hemorrhoid issues also seem more inclined to posterior prolapse.
“Friendly doctors and staff! Office was clean and comfortable. Doctor was caring and knowledgeable, taking time to really listen to me and answer all my questions.” - Katie Thigpen
200 Livingston Str,
Brooklyn, NY 11201
908 reviews
770 Flatbush Ave
Brooklyn, NY 11226
234 reviews
827 11th Ave
Manhattan, NY 10019
88 reviews
260 Ave X
Brooklyn, NY 11223
261 reviews
180 Myrtle Ave
Brooklyn, NY 11201
90 reviews
2315 3rd Ave
New York, NY 10035
40 reviews
Many non-invasive treatment options exist to manage your prolapse symptoms. After a pelvic exam and discussion of your medical history and current symptoms, your Brooklyn doctor may recommend:
If you need surgery, your gynecologist accesses your abdomen through your vagina. After removing the excess or stretched tissue, your doctor supports your pelvic organs with either sutures or a mesh patch that eventually integrates into the connective tissue or fascia between the rectum and the vagina. Recovery time for rectal surgery takes two to six weeks. Although less invasive than open abdominal surgery, your body still needs adequate time to heal and rest.
After recovery from rectocele surgery or as preventive steps against further posterior prolapse incidents, your Brooklyn gynecologist recommends a series of habit changes to support your pelvic floor muscles and keep you pain-free and healthy. These lifestyle recommendations include:
Posterior prolapse conditions cause discomfort, embarrassment and sometimes pain. Finding a solution to help control and treat your rectocele symptoms and concerns improves your quality of life, allowing you to do more and do it more easily. Treat your condition in a modern, safe environment. Contact doctor in Brooklyn at Century Medical and Dental Center for the best rectocele treatment.
Century Medical and Dental Center is an accredited healthcare facility in NY that operates in accordance with Article 28, a public health law. This law regulates and recognizes accreditation for public healthcare facilities, ensuring they are licensed and operated correctly. By undergoing the Article 28 process and achieving accreditation, Century Medical and Dental Center demonstrates its commitment to meeting the highest standards of care.
As a multidisciplinary medical center, we have highly qualified doctors, nurses, and support staff who are working hard to provide the best medical care to patients in Manhattan, NY, Brooklyn, NY, and Bronx, NY including Brooklyn Heights, Dumbo, Prospect Heights, Park Slope, Clinton Hill, Boerum Hill, Red Hook, Harlem, Gravesneck, Flatbush, and Bedford-Stuyvesant.